-
Phone
1300 17 44 97
-
Fax
02 8580 4867
-
-
Correspondence
Suite 1404, Level 14
St Vincent’s Private Hospital
406 Victoria Street
Darlinghurst NSW 2010
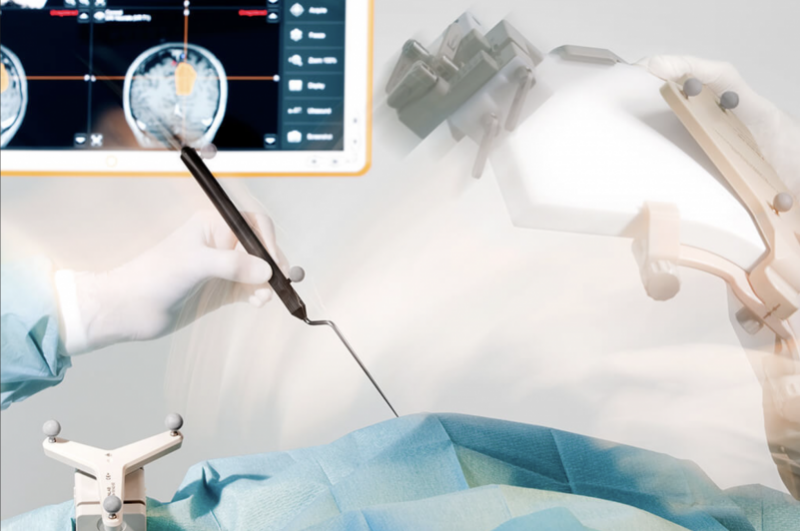
Automatic Image Registration for high precision MRI surgery with integrated intraoperative MRI scanner, courtesy BrainLab.
Intraoperative MRI (iMRI) is an advanced technology in which one or more MRI scans are performed during the surgery to determine whether the tumour resection is complete. Although all modern neurosurgery uses “navigation” systems, the brain usually shifts as a tumour resection is performed, making these navigation systems become less useful as the tumour resection proceeds. With the iMRI the navigation can be updated based on the images taken during the surgery to reduce the risk of errors.
In 2011 for the first time a Randomized Controlled Trial (these are the best type of evidence to support a treatment) was published comparing the completeness of resection when using an intraoperative MRI compared to resections without the MRI(1). Patients undergoing surgery with intraoperative MRI had complete resection 96% of the time, compared to only 68% in the standard operative group. There was no increased risk of neurological problems associated with the more complete resection.
There is now significant evidence available to suggest extent of resection correlates with survival in glioma surgery. Put in other words- the more tumour you remove the better the patient does.
Royal Prince Alfred Hospital in Sydney was the first hospital in Australia with an intraoperative MRI and currently has Australia’s largest experience with this technology. It remains the only hospital in NSW with this equipment.
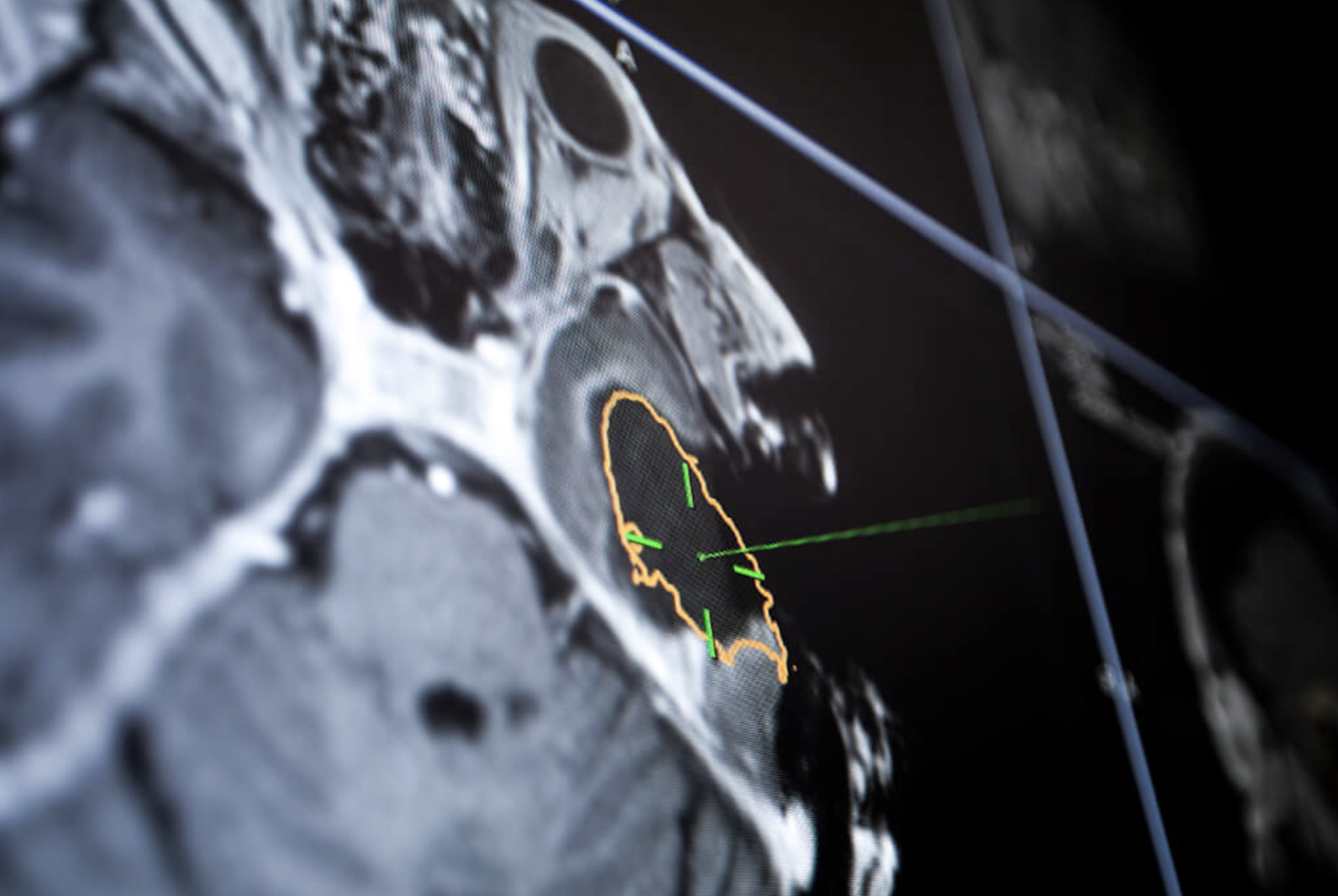
Integration of surgical navigation system enables MRI guided precision surgery, courtesy BrainLab.
1. Senft C, Bink A, Franz K, Vatter H, Gasser T, Seifert V. Intraoperative MRI guidance and extent of resection in glioma surgery: a randomised, controlled trial. Lancet Oncol. 2011 Oct;12(11):997–1003.