-
Phone
1300 17 44 97
-
Fax
02 8580 4867
-
-
Correspondence
Suite 1404, Level 14
St Vincent’s Private Hospital
406 Victoria Street
Darlinghurst NSW 2010
The diagnosis of a brain tumour can be a confronting time for patients and their families. It is difficult to give general advice concerning brain tumours, since there are many different different types of tumours often requiring different treatments and having different outcomes. Please consider this advice to be of a general nature and consult your neurosurgeon for specific advice concerning your own condition.

No. There are many different types of brain tumours and there are specific treatment options for each type which may include surgery, stereotactic radiosurgery and even observation with serial MRI’s. In some cases surgery is clearly the best option, but not always. It depends on many factors including patient symptoms, tumour location, how certain the diagnosis is based on the scan (and whether a sample needs to be taken to get a diagnosis), and how effective the alternatives are.
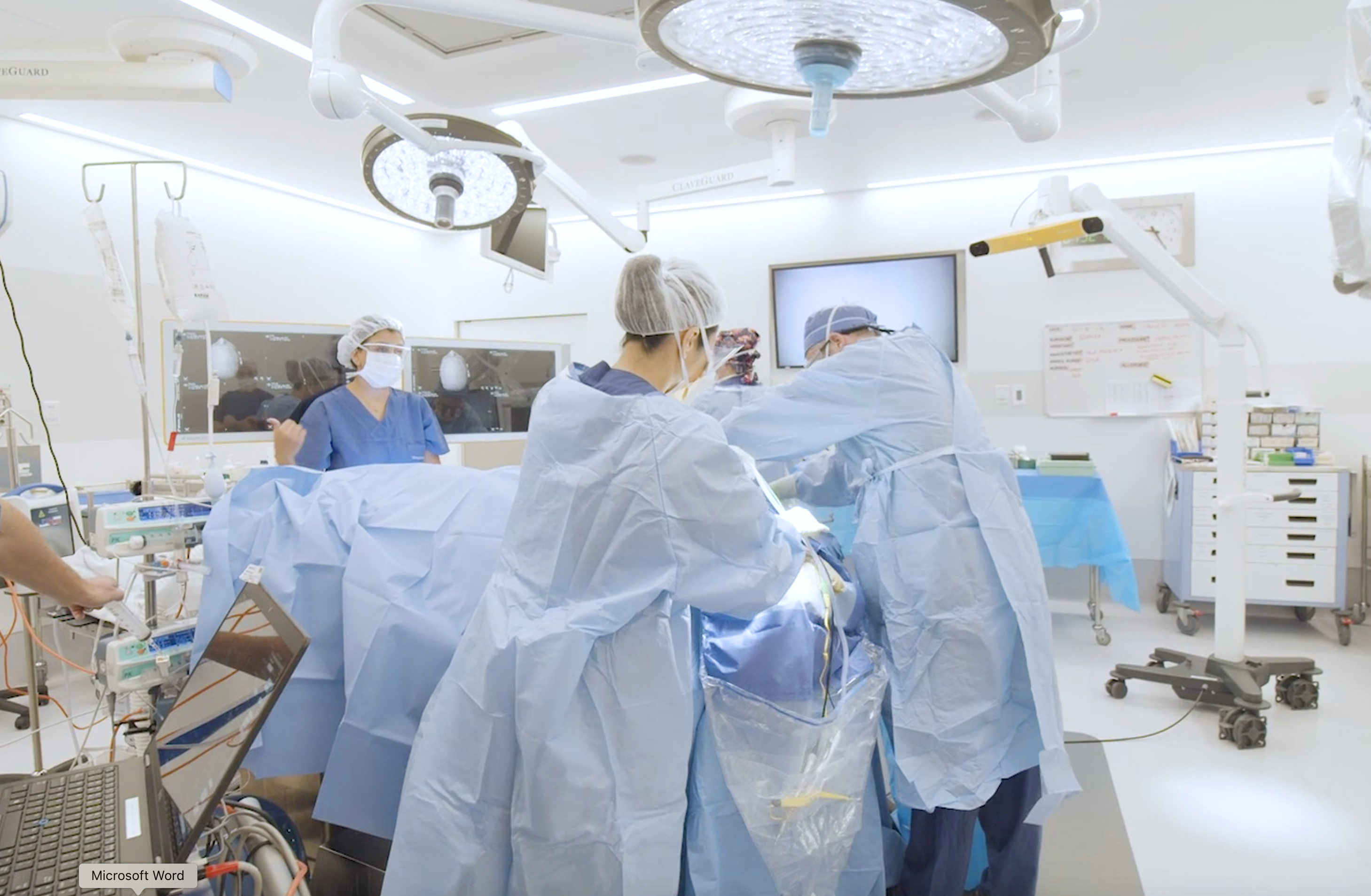
Intraoperative MRI is an advancement in neurosurgery which allows the patient to undergo one or more MRI scans during the operation to make certain that the tumour is completely removed. It may be surprising to learn that when an intraoperative MRI is not used – even in the best of hands – studies indicate around 30% of patients will have additional tumour even when the neurosurgeon thought the resection was complete. This technology takes the guesswork out of looking for residual tumour. Please see the intraoperative MRI information section of this website for more detail.
Patients with tumours that are close to the parts of their brain controlling language or movement may be recommended to undergo their surgery awake. Dr Jonker has a particular interest in this type of surgery in order to achieve maximal safe resection. The purpose of awake surgery is primarily to minimize the chance of causing a neurological complication such as paralysis or speech disturbance. It has been shown that patients with gliomas who sustain a neurological problem as a result of their surgery not only have a worse quality of life (as you might expect) but they also have a worse overall survival from their tumour(1).
Not every patient is suitable for awake surgery, and indeed it is not necessary for every patient. It is particularly useful for intrinsic brain tumours (especially low grade gliomas) located near the language areas.
Stereotactic radiosurgery is a technique developed by neurosurgeons to treat brain tumours, spine tumours and trigeminal neuralgia using highly focused radiation delivered precisely to the tumour, contoured to the shape of the tumour, and with minimal effect on the surrounding brain or other structures. It is usually delivered as a single treatment on one day. It is non-invasive and does not require admission to hospital. Treatments are done using technology such at the Novalis Tx Linear Accelerator and the Gamma Knife.
References
1. McGirt MJ, Mukherjee D, Chaichana KL, Than KD, Weingart JD, Quinones-Hinojosa A. Association of surgically acquired motor and language deficits on overall survival after resection of glioblastoma multiforme. Neurosurgery. 2009 Sep 1;65(3):463–9; discussion469–70.